A new study, published in Nutrients, looks at the profound effects of the gut-brain axis in both the formation and effects of eating disorders in women.
First off, the authors noted that, thanks to hormonal fluctuations, women are particularly biologically prone to developing eating disorders.
Second, the study looked at how changes to the microbacteria in the gut contribute to the formation of eating disorders, amplify their harmful consequences, and influence a bidirectional downward cycle of influence and outcome.
As in most other “mental” health issues, the composition of bacteria is absolutely profoundly important, and as I’ve mentioned ad nauseum, oh that more pastors would literally have a picture of the gut in their offices before going out an preaching sermons on mental health.
To the study:
Dr. Sanchari Sinha Dutta has a terrific read on it, so I’d urge you to go there if you want a fuller read on this, but essentially – we know that the human body, for many reasons, experiences alterations to its gut bacteria.
For women, the role of hormones is particularly powerful, which may explain why they’re more likely to develop eating disorders.
But viral illness, bacterial illness, parasitic infections, antibiotics – these all clearly affect our gut bacteria. As can other things – like sleep disturbances, stress (which often is amplified by altered gut bacteria itself!), diet, just life things that happen.
Those gut changes affect our brain. Brain stuff then affects the gut. So the relationship is bidrectional and it’s not always clear what comes first – the bacterial change or what’s going on in the brain. But it’s safe to say that our gut bacteria is always changing.
Now, it can change in such a way that it sets off a deleterious chain of events that lead to the formation of all kinds of sicknesses, including eating disorders.
Dr. Dutta writes more of how this happens:
Emerging evidence highlights a multifactorial crosstalk between immune–inflammatory pathways, disordered eating behaviors, and mood-related psychopathology. In patients with anorexia nervosa, a reduced abundance of short-chain fatty acid (SCFA)- producing bacteria has been observed. This disrupts intestinal permeability and facilitates the blood’s translocation of microbes and microbial metabolites. This cascade subsequently increases pro-inflammatory cytokine levels and impacts neuroimmune signaling and brain functioning.
Gut microbiota-derived SCFAs are crucial in regulating appetite and maintaining metabolic homeostasis by increasing satiety hormones leptin, glucagon-like peptide-1 (GLP-1), and peptide YY.
SCFAs primarily influence brain activities by altering neuroinflammation, promoting microglial maturation, and regulating the synthesis of neurotransmitters and neurotrophic factors. Inflammatory activity in the brain has been found to increase anorexia nervosa risk by suppressing the appetite-stimulating hormone ghrelin, leading to early satiety and reduced food intake. However, evidence also suggests that SCFAs may have context-dependent effects on appetite and behavior, influenced by dietary composition, microbial taxa, and host physiology.
Now… if you read all that, it’s impossible to cast stones at folks for developing eating disorders — just as it is for any other “mental” illness, which science has shown are clearly physical illnesses.
Again, we don’t blame someone’s spirituality for their cancer, and just as emphatically, we should reject spirituality as cause for “mental” illness. In fact, to do so, is taking something sacred (pain) and desecrating it. Jesus never did that to anyone in any kind of pain and neither should the church.
Back to the study…
The potentially good news arising from this study is that much better help for those with eating disorders may be on the way, thanks to discoveries like these.
Scientists are now working on developing microbiota-targeted interventions for helping restore a normal gut microbiota in victims of the disease.
This includes specific probiotics, prebiotics, targeted dietary shifts (everyone has different deficiencies and needs in their diets), and fecal microbiota transplantation (FMT).
Each of those may be more effective than current treatment by really getting to, well, the gut of the problem.
Finally, I want to say this.
Without minimizing other “mental” illnesses that get a lot of attention (depression, anxiety, PTSD, OCD), eating disorders are empirically the most physically dangerous, and absolutely wreak havoc on an individual’s mind and body. In fact, they’re often associated with developing those other diseases, as well.
The interesting thing is that a common Christian answer to the problem of eating disorders is “clean eating.” In fact, if you look at the culture right now, “clean eating” is all the rage for an answer to everything.
It’s good to eat healthy, but my concern is the way “clean eating” is currently often being linked to our bodies being temples of the Holy Spirit, and an overemphasis on clean eating is proven to be a risk factor for “orthorexia,” which is the gateway condition for a whole multitude of eating disorders.
I wrote an extensive piece on this and why the Christian community might be particularly prone to advancing this.
One of the way is just how tragically the sin of “gluttony” has been reframed as “eating a lot of junk food” when gluttony had absolutely nothing to do with “eating a lot” in the Bible.
You can read that piece here.
Finally, some resources.
To start with — some resources.
The National Institute of Mental Health on eating disorders, including signs, symptoms, risk factors, treatments and help.
A 24/7 hotline for those struggling with eating disorders or any other mental health disorder.
Six Common Types of Eating Disorders.
And find an eating disorder therapist near you.
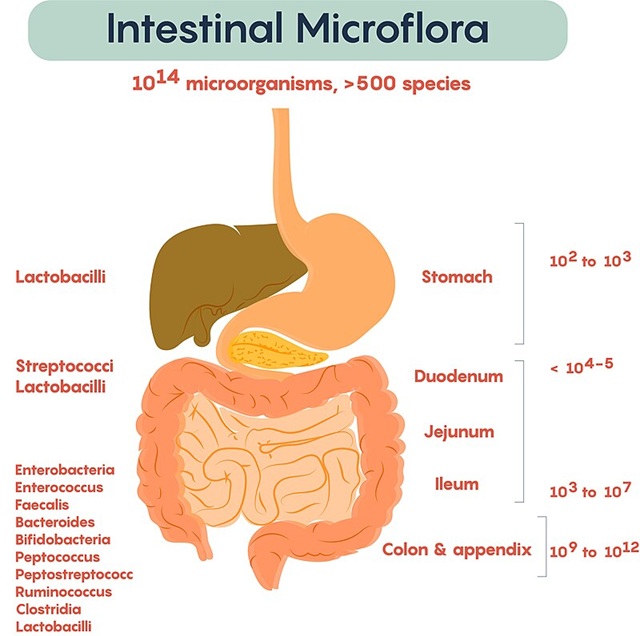
[Photo: Composition and distribution of intestinal microflora by Dr. William Ju, University of Toronto, via Wikipedia]